Three Commonly Misdiagnosed Retinal Conditions

It can be difficult for doctors and patients alike to understand why a medical misdiagnosis has taken place. However, there are many reasons why an incorrect diagnosis could occur. One reason is that there are countless medical conditions that can closely mirror one another – even to such a degree that a trained and experienced medical professional with advanced diagnostic equipment could choose one condition over the correct issue.
One of the ways the medical industry (including the field of retina care) works to reduce instances of misdiagnoses is to better educate the community, particularly in cases where the condition is well known for being misdiagnosed. At Austin Retina Associates, we want to ensure that our doctors are armed with all available knowledge for patient care and that patients can feel confident in the decisions their doctors are making.
Three Commonly Misdiagnosed Retinal Conditions
Macular Hole
Often, patients who are referred to our practice by another doctor have been told that they have a macular hole, but what they actually have is a lamellar macular hole. The reason the two conditions are confused is that a macular hole is simply a more severe version of a lamellar macular hole. To further illustrate:
- A macular hole extends through all of the retina layers; a lamellar macular hole does not.
- A macular hole requires surgical treatment; a lamellar macular hole usually isn’t treated with surgery unless the patient’s vision worsens.
Retinoschisis
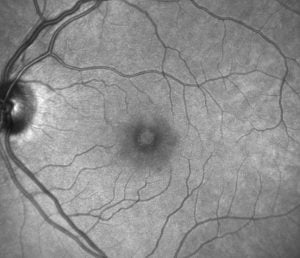
Central Retinal Vein Occlusion