About Retinopathy of Prematurity (ROP)
Retinopathy of prematurity (ROP) is a potentially blinding eye disorder that primarily affects premature infants weighing 1500 grams or less that are born before 32 weeks of gestation (A full-term pregnancy has a gestation of 38–42 weeks). The smaller a baby is at birth, the more likely that baby is to develop ROP. This disorder—which usually develops in both eyes—is one of the most common causes of visual loss in childhood and can lead to lifelong vision impairment and blindness.
There are approximately 3.9 million infants born in the U.S. each year. About 14,000 are affected by ROP and 90% of those affected have only mild disease. About 1,100- 1,500 develop disease severe enough to require medical treatment and 400-600 infants each year in the U.S. become legally blind from ROP.
We treat Retinopathy of Prematurity (ROP) at all of our locations.
To schedule an appointment, please call us or fill out our online form.
What causes ROP?
Several complex factors may be responsible for the development of ROP. The eye starts to develop at about 16 weeks of pregnancy, when the blood vessels of the retina begin to form at the optic nerve in the back of the eye. The blood vessels grow gradually toward the edges of the developing retina, supplying oxygen and nutrients. During the last 12 weeks of a pregnancy, the eye develops rapidly. When a baby is born full-term, the retinal blood vessel growth is mostly complete (The retina usually finishes growing a few weeks to a month after birth). But if a baby is born prematurely, before these blood vessels have reached the edges of the retina, normal vessel growth may stop. The edges of the retina, the periphery, may not get enough oxygen and nutrients.
In addition to birth weight and gestational age, other factors that are associated with the presence of ROP include anemia, poor weight gain, blood transfusion, respiratory distress, breathing difficulties and the overall health of the infant.
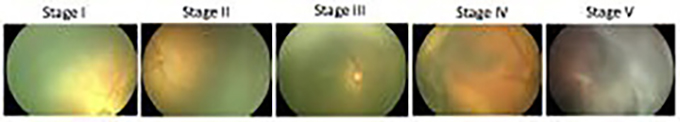
Stages of ROP
Mildly abnormal blood vessel growth. Many children who develop stage I improve with no treatment and eventually develop normal vision. The disease resolves on its own without further progression.
How is ROP Treated?
The most effective proven treatments for ROP are injections of medication or laser therapy. Injections are performed under sterile conditions to limit risk of infection. Use of a small volume syringe allows for good hand control throughout the procedure, which is a key factor when injecting small eyes under topical anesthesia with unpredictable cooperation. Laser therapy “burns away” the periphery of the retina, slowing or reversing the abnormal growth of blood vessels. Unfortunately, the laser treatment can also destroy some side vision. This is done to save the most important part of our sight – the sharp, central vision we need for “straight ahead” activities such as reading, sewing, and driving.
Scleral buckle
This involves placing a silicone band around the eye and tightening it. This keeps the vitreous gel from pulling on the scar tissue and allows the retina to flatten back down onto the wall of the eye. Infants who have had a scleral buckle need to have the band removed months or years later, since the eye continues to grow; otherwise they will become nearsighted. Sclera buckles are usually performed on infants with stage IV or V.
Vitrectomy
Vitrectomy involves removing the vitreous and replacing it with a saline solution.
After the vitreous has been removed, the scar tissue on the retina can be peeled back or cut away, allowing the retina to relax and lay back down against the eye wall. Vitrectomy is performed only at stage V.
Why are eye exams recommended after discharge from the hospital?
It is critical to have eye exams after discharge from the hospital since ROP may not be resolved before discharge. Also, even with successful treatment of ROP, prematurity may lead to other vision abnormalities such as the development of amblyopia (lazy eye), eye misalignment (strabismus), the need for glasses (even at a young age), and cortical visual impairment. Therefore, every premature infant needs the long-term attention of an ophthalmologist.
For Retinopathy of prematurity treatment in Austin, Texas, call 800-252-8259.
For additional information, please visit the ASRS page on Retinopathy of prematurity.